Risks of ECV vs C Section & Which Procedure is Best for You
If your baby is breech after 36 weeks, you have three options: coax that stubborn baby to turn naturally, have a doctor perform an external cephalic version (ECV), or schedule a c-section. When I found out that my baby was breech, I struggled with this decision. To me, it seemed like there were just as many risks associated with ECV procedures as c-sections. It made choosing between the two impossible.
Do you feel the same? I get it. I totally get it. That’s why I wrote this post. In it, we’re going to compare the benefits and risks of both procedures. Before we begin, I want to give you a disclaimer: I am a mom of two breech babies, but that’s it. I’m not a medical professional. I’m not a consultant. I’ve researched this topic extensively, but keep in mind that this post is also based on my experiences and opinions. I think seeking out another person’s unique insights is valuable when you’re facing a difficult decision, but you may not agree. That’s okay.
POSTS RELATED TO RISKS OF ECV VS C SECTION:
- What is a Breech Baby: Breech Presentations, Complications, Etc.
- What to Do When Your Baby is Breech: Your Breech Pregnancy Step-by-Step Guide
- 10 Ways to Turn a Breech Baby Naturally
- Is it Safe to Have a Vaginal Breech Birth?
- Is an External Cephalic Versions Worth It?
When I found out that my firstborn was breech, I was completely floored. It felt like all of my dreams for a perfect labor (whatever that is) had died in an instant. And, honestly, I was scared. The whole birthing process seemed terrifying anyway.
There was a lot of information out there about breech presentations, but I found it vastly overwhelming. For my second breech pregnancy, I was prepared. I knew the facts, I’d experienced this scenario before. I was ready.
That’s why I wrote these blog posts. I want to help other moms and moms-to-be to understand what having a breech presentation means and what options are available to you.
Because knowledge = confidence.
For my first pregnancy, I decided to go with a planned caesarean section. For my second pregnancy, I decided to schedule an ecv procedure. I get into why in this post here. The thing is, there’s risks associated with ecvs. There’s risks associated with cesereans. Your decision will be based on your particular situation. That’s why we’re detailing all of those facts out in this post.
Advantages of an External Cephalic Version
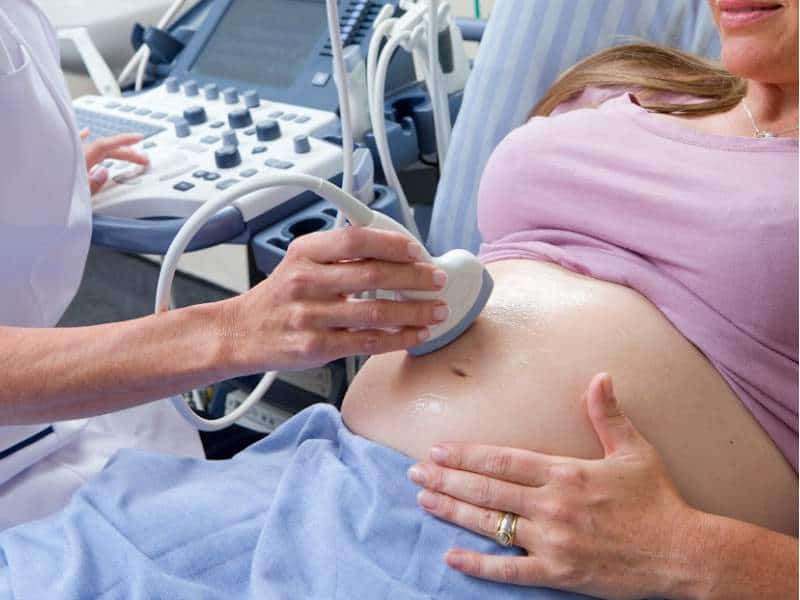
An ECV attempts to turn a breech baby manually. At the beginning of the procedure, the doctor will generally administer terbutaline to prevent early labor, confirm the baby’s position with an ultrasound, and palpitate for your baby’s little booty and head. An ECV is safe for most women and babies and considered a noninvasive.
The caveat is, an In addition, some mothers worry about the safety of the baby and the chance of a reversion at a later date. Let’s dig into these facts a little.
ECVs are Non-Invasive Procedures
The longest part is waiting. Usually, the actual procedure is about 15 minutes. Your doctor will gently move your baby from your pelvis, rotate his little body head-down, and then you’re done. There’s a video on Youtube that actually shows how easily a successful, no-drama ecv is performed.
ECV Success Rates are Good
The success rate of external cephalic versions is about 60%. When I first heard that statistic, I grimaced. I mean, that’s a 40% failure rate, right?
But listen. The success of ECVs has to do with these factors:
- Your baby’s presentation. A frank breech position has a less likely chance of success.
- Your BMI–the greater the BMI the greater the risk.
- Gestation: 37 weeks is the magic window of opportunity for a successful ECV.
- Amniotic fluid: According to this study, an ample amount of amniotic fluid is correlated to a high ECV success rate.
- Practitioner: I couldn’t find any studies on this, but to me (and this is my opinion) your practitioner should feel very comfortable and experienced if they’re going to perform an ECV. This is largely why I decided to have an ECV performed for my second pregnancy. My doctor had successfully completed several procedures and felt very confident with it.
Increased Chance of a Vaginal Delivery
This was another huge determining factor me to select an ECV during my second pregnancy. I desperately wanted to have a natural birth. My first delivery sucked. It was literally 31 hours of torture (okay, 19 hours of torture, and the rest was an epidural-induced daze).
And, with a toddler at home, I hated the idea of spending days in bed recovering from a cesearean. Don’t get me wrong, c-sections are life-saving procedures and I’m totally grateful for them. I just wanted to avoid one if at all possible.
An ECV significantly lowers the risk of cesareans. According to this study, 75% of the women who had a successful external cephalic version went on to give birth vaginally.
Minimal Recovery Time
My doctor told me that most women can leave the hospital that day with minimal soreness. Heck, yeah.
Assuming your doctor was able to turn the baby, you’ll stay at the hospital for a couple hours to monitor the fetal heart rate and your vital signs. Then, you just wait until your little one decides to come.
Risks of ECVs
40% Failure Rate
The fact is, if you attempt an ECV, it may not be successful. Sometimes, there’s not enough amniotic fluid for your baby to move around. Sometimes, your doctor will see signs of fetal distress and stop the procedure altogether. When I asked my doctor about this, she said that it’s very rare. The most likely hindrance she saw was that baby simply wouldn’t move.
Experience on How to Perform ECV May Vary
Personally, I think the success of external cephalic versions hedges on the experience of your provider. How many ECVs have they successfully performed. How many unsuccessful ECVs have they seen?
Do they feel comfortable doing it in your situation? If not, I would get a second opinion. See if they have a peer that has more experience with this type of procedure.
Risks to the Fetus (Although Small)
The risk of a complication in an ECV is about 1%.
Here are some that you should consider:
- Placental abruption–This was my biggest fear, even if it is very rare (less than .12%).
- Cord twists
- Membrane rupture
- Fetal distress. According to another study, a baby’s heart rate might pick up during the operation, but return to normal once it is over.
- Fetal Risks Associated with Terbutaline
- ECV May Result in An Emergency Cesarean Section
It’s a decently small risk, but some studies indicate that the risk of an emergency c-section is about .5%.
Baby Could Revert to the Breech Position
This happens about 5% of the time. It really depends on your amniotic fluid levels, the baby’s size, your weeks of gestation, and how stubborn your little guy is.
Benefits and Risks of Cesarean
If you decide to opt out of an ECV (or experience an unsuccessful ECV) and still have a breech presentation at term, you’ll need to schedule a c-section. That will be the safest way to give birth to your baby.
When my doctor suggested a planned cesarean, I felt like a failure. I’d never considered a c-section; Oddly enough, giving birth was kind of a bragging point for my family. So, I would have been the only woman in my family to have a c-section.
Not to mention, all of my hopes and dreams of having a wonderful, natural birth went down the toilet.
If you find yourself feeling the same way, STOP! The important part of the birthing process–the truly important part–is you and your baby. Your birth story will be beautiful, no matter how you do it.
With that said, let’s take a look at some of the risks and benefits of this procedure. Unlike emergency c-sections, a planned cesarean is usually quite laid back and decently convenient. You know
Like most things attached to motherhood, these preconceptions are ridiculous. Planned c-sections are SO low-key, extremely convenient, offer many of the same advantages as a natural birth, and in no way reflect your birthing success.
Convenience
After I decided to plan a cesarean, I was struck by how convenient it felt. My husband could take off work. We didn’t have to worry about when the baby would come or if we were prepared. We simply showed up at the hospital, prepped my body, and waited.
My doctor also suggested a “Gentle C-Section” or “Patient-Centered C-Section”; This focuses on the natural aspects of birth, such as immediate skin-to-skin, delayed cord-clamping, immediate breastfeeding etc. Many doctors are willing to make these accommodations as long as the infant is safe.
Of course, my baby threw all that out the window when a last-minute ultrasound revealed that she had flipped the night before.
Now, to be completely realistic, the recovery of a c-section is not convenient. But, the scheduling is!
Decreased Risks for Baby
With an ECV, the risks of complications are small, but still there. With a c-section, the most common injury (which sits at 1%) is a skin laceration.
You May Be Able to Have a VBAC Next Time
If you have a breech presentation with one pregnancy, the risk of a breech presentation with the next is higher.
Many women go on to have a vaginal birth after c-sections (VBAC). So, if you decide that a c-section is the best option for your situation right now, you may still be able to have a vaginal birth during the next pregnancy.
I knew that many factors were stacked against me for this pregnancy, making the ECV less likely to work. However, the hope that I might be able to have a vaginal birth with the next one encouraged me.
Here’s a cool statistic, Mama. Women who elect to have a planned c-section the first time are 50% more likely to have a successful VBAC the next time around, compared to say another complication (like a uterine rupture). It is possible!
Risks of a C-Section
For Baby
The dangers to the baby are few (about 1% chance of a complication). The most common injury is a skin laceration. Your baby may show a low APGAR score. This is the case for about 50% of babies born via cesarean. This is a quick test performed within the first five minutes of your baby’s life.
It rates the following on a scale between 0-2:
- Breathing
- Heart rate
- skin color (for example, purple vs pink hue)
- Your baby’s reflexes
A baby with a score lower than 7 needs additional medical attention.
For Mother
A c-section, even planned, is a major surgical procedure. A surgeon will cut through your abdominal wall and uterus. You’ll need time to heal, and it may affect every future pregnancy. Here are a few risks you should consider before you decide against trying an ECV.
- Maternal mortality rate is higher than vaginal births.
- Small increased risk of severe postpartum complications, such as infections or blood clots.
- Longer recovery rate— 3-5 days in the hospital, extended home recovery with physical limitations.
- Other c-section related risks, such as accidental incisions and additional surgeries.
- Future VBAC complications (less than 1% risk for a uterine rupture)
- More likely to have c-section in the future (however, the same applies to breech pregnancies, according to some studies)
Final Thoughts on an External Cephalic Version vs C-section for Breech Babies
As you can tell, this is not a cut and dry comparison. Both procedures have low complication rates and both are considered safe for you and your baby.
Whichever procedure you opt for, be confident that you are making the right decision for your child. Speak with other women about both procedures, and have multiple conversations with your doctor.
Many moms have so many different feelings about both procedures, so I want to encourage you that there is no “right” or “wrong” decision here. Do what’s best for you and your little one!
On a final note, if you’re nearing D-Day, don’t lose hope. You can still turn that baby around. I did! If you want to know how I turned my baby at 39 weeks, check out my earlier post, How to Turn a Breech After 36 Weeks.
Veteran moms, if you had a breech baby or if your ECV was successful (or unsuccessful!) let us know in the comments below! We’d love to hear all experiences of attempted external cephalic versions. You never know what might be helpful to another mama.






